What if your doctor told you that you’re developing a serious chronic condition, but you still have time to completely prevent it? Would you take immediate action, or would you wait until the condition becomes permanent? For the 96 million American adults with prediabetes, this isn’t a hypothetical scenario—it’s a critical reality that most don’t even realize they’re facing.
Have you ever wondered why some people with elevated blood sugar are told they can potentially reverse their condition, while others are prescribed medication they’ll likely need for life? The answer lies in understanding the fundamental difference between prediabetes and diabetes—a distinction that goes far beyond simple blood sugar numbers to the cellular level where your metabolic health is determined.
When exactly does your body cross the line from reversible metabolic dysfunction to permanent damage? How can you recognize the often-subtle warning signs that you’re approaching this critical threshold? Why do standard medical tests frequently miss prediabetes until it’s already transitioned to diabetes? And most importantly, what specific actions can you take if you find yourself in the reversible stage?
At IFitCenter, these questions represent the foundation of our approach to metabolic health. In this comprehensive guide, we’ll provide clear, evidence-based answers about the difference between prediabetes and diabetes, empowering you with the knowledge to identify which side of this critical boundary you’re on and what steps you can take to protect your long-term health.
The Common Origin: Understanding Blood Sugar Regulation and Metabolic Dysfunction
The Glucose-Insulin Relationship: How Your Body Manages Blood Sugar
Your body’s blood sugar system works like a carefully balanced equation. You have approximately one teaspoon of sugar circulating in your bloodstream at any given time—just enough to fuel your cells but not enough to cause harm.
When you eat carbohydrates (bread, pasta, fruit, or sweets), they break down into glucose and enter your bloodstream. Your pancreas responds by releasing insulin, which acts like a key, unlocking your cells so glucose can enter and be used for energy.
In a healthy system, this process is nearly seamless. You eat, glucose levels rise temporarily, insulin responds appropriately, and your blood sugar returns to normal within hours.
But this system can gradually break down. When we consistently consume more carbohydrates than needed, our cells become overwhelmed by the constant influx of insulin—the beginning of insulin resistance.
Think of insulin resistance like developing selective hearing. Your cells start to “ignore” insulin’s signals, forcing your pancreas to release more and more insulin to accomplish the same task.
Several modern lifestyle factors contribute to this problem: diets high in processed carbohydrates, sedentary behavior, chronic stress, and poor sleep patterns all disrupt healthy glucose regulation.
The Metabolic Continuum: From Normal Metabolism to Diabetes
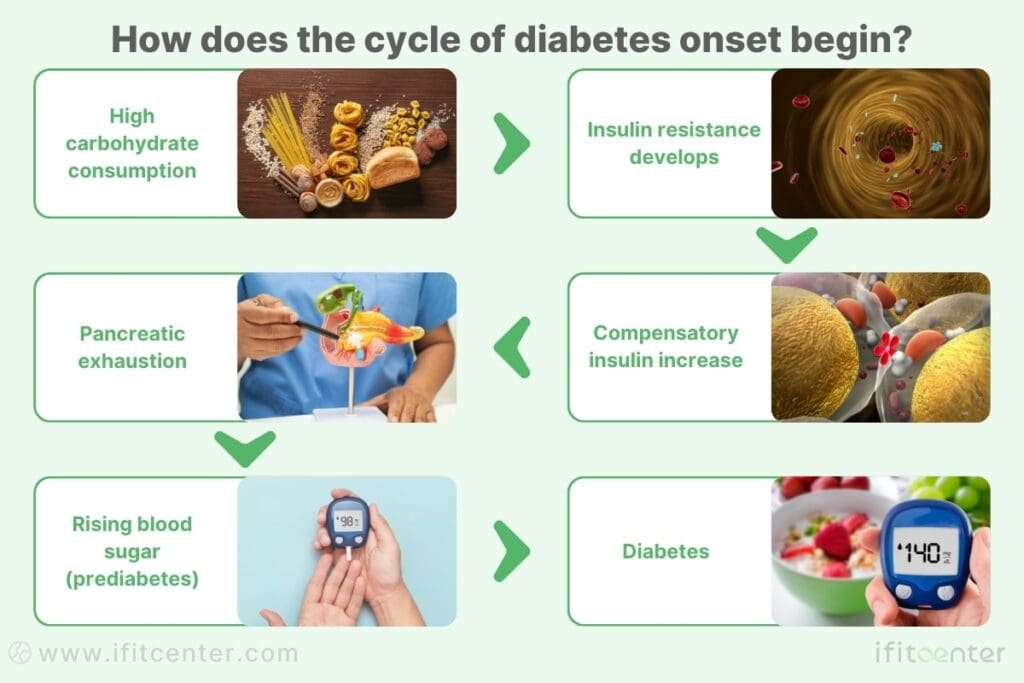
The journey from normal metabolism to diabetes follows a predictable pattern that typically unfolds over 10-15 years. Understanding this progression reveals why prediabetes and diabetes are fundamentally different conditions.
- High carbohydrate consumption leads to elevated insulin: The average person consumes about 31 teaspoons of sugar equivalent daily, forcing the body to produce extra insulin to manage this load.
- Insulin resistance develops: Your cells begin putting up barriers against the constant flood of insulin as a protective mechanism.
- Compensatory insulin increase: Your pancreas produces even more insulin to overcome this resistance. People with insulin resistance often have 5-7 times more insulin in their bloodstream than normal.
- Pancreatic exhaustion: After years of overwork, the insulin-producing beta cells in your pancreas become exhausted but are not yet permanently damaged.
- Rising blood sugar: As insulin production can no longer keep up with demand, blood glucose levels begin to rise, first into the prediabetic range and eventually into diabetic territory.
This progression is like pushing your car’s engine too hard for too long. Initially, the car compensates, but eventually, performance declines as components wear out.
The 10-15 year progression timeline offers a substantial window for intervention. Most people are diagnosed with prediabetes when they’re already in stage 3 or 4, but catching it early dramatically improves outcomes.
The Critical Difference Between diabetes and prediabetes
Prediabetes: The Reversible Stage of Metabolic Dysfunction
Prediabetes represents a critical metabolic crossroads. At its core, prediabetes is characterized by insulin resistance combined with a compensatory increase in insulin production—but crucially, without permanent damage to the pancreatic β-cells that produce insulin.
During prediabetes, your body’s cells resist insulin’s signals, but your pancreas responds by working overtime. Imagine a factory where the workers (your cells) are ignoring instructions, so the manager (your pancreas) keeps sending more and more messages to get the same work done. The workers are still functional, and the manager is exhausted but not permanently impaired.
What makes prediabetes reversible? The key lies in the state of your pancreatic β-cells. These specialized cells produce insulin in response to rising blood sugar. In prediabetes, these cells are stressed and overworked, but they haven’t sustained permanent damage. They’re like muscles that have been overexerted—they need rest and recovery, not replacement.
This distinction is crucial to understand. The cellular changes in prediabetes include:
- Reduced insulin sensitivity in muscle, liver, and fat cells
- Increased demand on pancreatic β-cells to produce insulin
- Mild elevation in blood glucose levels
- Temporary reduction in first-phase insulin response
- Reversible β-cell dysfunction without significant cell death
Think of prediabetes like a car engine that’s been running too hot for too long. The engine is strained and performing poorly, but if you address the underlying issues—perhaps cooling it down and changing the oil—it can return to normal function. Similarly, with appropriate intervention, the metabolic changes of prediabetes can be reversed, and normal glucose regulation can be restored.
Diabetes: When Pancreatic Damage Becomes Permanent
Diabetes marks the point where metabolic dysfunction crosses a critical threshold into irreversibility. The defining feature of type 2 diabetes is not just insulin resistance—which is also present in prediabetes—but the permanent damage to pancreatic β-cells that prevents adequate insulin production.
Continuing our factory analogy, diabetes occurs when the manager (pancreas) has not only become exhausted but has actually lost the capacity to send sufficient messages. No matter how hard the pancreas tries, it simply cannot produce enough insulin to overcome the resistance. The factory’s communication system has suffered permanent damage.
The physiological changes that make diabetes irreversible include:
- Substantial β-cell death (studies suggest 40-60% of β-cells are lost by diagnosis)
- Amyloid deposits in the pancreas that disrupt remaining β-cell function
- Chronic inflammation that continues to damage pancreatic tissue
- Mitochondrial dysfunction within remaining β-cells
- Impaired insulin gene expression
Returning to our car analogy, diabetes is like an engine that has experienced mechanical failure. Parts have broken, metal has warped, and simply cooling it down won’t restore function. Some components need replacement, and others will never work properly again.
This permanent damage fundamentally changes treatment goals and approaches. While prediabetes treatment focuses on restoring normal function, diabetes management aims to compensate for lost function through:
- Medications that stimulate remaining β-cells to produce more insulin
- Drugs that reduce glucose production by the liver
- Therapies that increase insulin sensitivity in target tissues
- External insulin supplementation when necessary
Understanding this irreversibility underscores why prevention is so critical. Once the threshold into diabetes is crossed, complete restoration of normal glucose metabolism becomes impossible with current medical capabilities. Management replaces cure as the primary goal.
“What many of my patients find most surprising is that insulin resistance itself isn’t the fundamental difference between prediabetes and diabetes—it’s present in both conditions. The critical distinction lies in β-cell function. In prediabetes, these insulin-producing cells are stressed and overworked but still capable of recovery, while diabetes represents the point where a significant portion of these cells have been permanently damaged. This explains why lifestyle interventions that reduce the demand on these cells can potentially reverse prediabetes, yet can only manage, not cure, diabetes.”
Dr. Babak Jamalian, Family Physician.
To read more about prediabetes, I strongly recommend using the following links:
- What is Prediabetes?
- Can Diabetes Be Cured?
- Signs and Symptoms of Prediabetes
- The Connection Between Obesity and Prediabetes
- Can Prediabetes Be Reversed?
- How to Diagnosis Prediabetes?
- Foods to avoid in prediabetes
- Prediabetes Reversal Through Weight Management
- Insulin Resistance and Diabetes
The Window of Opportunity: Why Early Intervention Matters
The reversibility of prediabetes creates a critical window of opportunity for intervention. Research demonstrates that this window is both real and significant—but it doesn’t remain open indefinitely.
The scientific evidence supporting prediabetes reversal is compelling. The landmark Diabetes Prevention Program (DPP) found that intensive lifestyle changes reduced progression to diabetes by 58% over three years. A follow-up study showed these benefits persisted, with a 34% reduction in diabetes incidence over 10 years compared to placebo groups.
These aren’t small improvements—they represent life-changing differences. According to studies published in Diabetes Care, approximately 5-10% of people with prediabetes progress to diabetes annually without intervention. However, with appropriate lifestyle changes, 14-59% can actually revert to normal glucose regulation within 3-5 years.
Several factors influence your personal reversibility potential:
- Duration of prediabetes: The longer you’ve had elevated blood sugar, the more β-cell function may be compromised
- Degree of insulin resistance: More severe resistance requires more aggressive intervention
- Genetic factors: Family history affects both progression risk and response to interventions
- Age: Younger individuals typically have greater capacity for β-cell recovery
- Body composition: Visceral fat accumulation particularly impacts reversibility
Perhaps most importantly, research indicates that this window of opportunity has a limited timeframe. Studies suggest that the most effective intervention occurs within the first 3-5 years after developing prediabetes. As time passes, the likelihood of successful reversal gradually diminishes.
This doesn’t mean later intervention is futile—improvements can still be made at any stage. But the potential for complete reversal decreases as β-cells experience prolonged stress and begin to sustain permanent damage.
Think of prediabetes as a metabolic fire alarm. It’s not the fire itself (diabetes), but the warning that a fire is imminent. Responding to this alarm promptly can prevent permanent damage. Ignoring it doesn’t change the risk—it only allows the situation to deteriorate while the opportunity for prevention gradually slips away.
“The most telling prediabetes symptom I observe in clinical practice is what I call ‘cellular hunger’—patients who eat regular meals yet still experience persistent hunger, particularly for carbohydrates. This occurs because insulin resistance creates a situation where cells cannot efficiently access glucose despite adequate levels in the bloodstream. The body responds by triggering hunger signals, especially for quick energy sources. When patients report feeling unsatisfied after meals or needing to snack frequently throughout the day, it’s not a willpower issue—it’s a metabolic signal we should recognize as a potential warning sign.”
Dr. Babak Jamalian, Family Physician.
I am making a completely scientific picture. The ones I have are in Persian. Please translate any text I send you into English, observing all the rules of English spelling and grammar.
- Best Fruits for Diabetic Patients
- Superfoods for control Blood Sugar
- Is Diabetes Genetic?
- What is HbA1c Test?
Reverse Prediabetes at IFitCenter Before It’s Too Late
The difference between prediabetes and diabetes isn’t just about blood sugar levels—it’s about time. Prediabetes is reversible, but once your body crosses the threshold into diabetes, the damage is permanent. Weight loss isn’t just about appearance—it’s a medical strategy for restoring insulin sensitivity and protecting your pancreas from long-term harm.
At IFitCenter, our physician-supervised weight loss program is designed to:
✅ Lower insulin resistance by targeting fat accumulation
✅ Enhance metabolic health through structured nutrition and medical oversight
✅ Provide continuous monitoring to ensure safe and effective weight reduction
Time is the deciding factor. Start today to ensure you stay in control of your health.
Summary and Action Steps: Taking Control of Your Metabolic Health
Throughout this article, we’ve explored the critical distinction between prediabetes and diabetes—a difference that goes far beyond simple blood sugar numbers to the cellular level where your metabolic health is determined. Let’s reinforce this fundamental difference before discussing practical steps you can take today.
Prediabetes represents a state of metabolic stress where your pancreatic β-cells are overworked but still functional. Like an athlete who’s been pushed too hard, they need recovery time, not replacement. With appropriate intervention, these cells can regain normal function, and proper glucose regulation can be restored.
Diabetes, by contrast, involves permanent damage to these insulin-producing cells. Studies show that by the time diabetes is diagnosed, approximately 40-60% of β-cells have already been lost—a level of damage that cannot be fully reversed with current medical capabilities.
Understanding this distinction transforms how we approach elevated blood sugar. Prediabetes isn’t just a warning sign—it’s a critical window of opportunity where appropriate action can potentially prevent a lifetime of managing a chronic condition.
To access other content on the IFitCenter’s blog, you can use the following links:
References
- American Diabetes Association. Standards of Care in Diabetes—2025. Diabetes Care. 2025.
https://diabetes.org/newsroom/press-releases/american-diabetes-association-releases-standards-care-diabetes-2025 - Bellary S, Kyrou I, Brown JE, Bailey CJ. Comprehensive Analysis of Screening for Diabetes and Prediabetes and their Prediction. Diabetes Metab Syndr. 2021;15(4):102235.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8375583/ - Tabák AG, Herder C, Rathmann W, Brunner EJ, Kivimäki M. Pre-Diabetes and What It Means: The Epidemiological Evidence. Annu Rev Public Health. 2021;42:59-77.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8026645/ - Prentki M, Nolan CJ. Islet β cell failure in type 2 diabetes. J Clin Invest. 2006;116(7):1802-1812.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1483155/ - Lowell BB, Shulman GI. Mitochondrial dysfunction and type 2 diabetes. Science. 2005;307(5708):384-387.
https://joe.bioscientifica.com/view/journals/joe/236/3/JOE-17-0367.xml - Gonzalez-Franquesa A, Patti ME. Insulin resistance and mitochondrial dysfunction. Adv Exp Med Biol. 2017;982:465-520.
https://pubmed.ncbi.nlm.nih.gov/28551798/ - Muoio DM, Newgard CB. Mechanisms of disease: molecular and metabolic mechanisms of insulin resistance and beta-cell failure in type 2 diabetes. Nat Rev Mol Cell Biol. 2008;9(3):193-205.
https://pubmed.ncbi.nlm.nih.gov/18200017/



